Dizziness: A Physical Therapy Perspective
Dizziness & Vertigo: What we learned from our physical therapists and PT assistant at Langford.
For those of you who attended our dizziness workshop in September, thank you! We are so glad we get to share our knowledge with our community. For those of you who missed it, here is a recap from our very own Dr. Karen Lovely, PT, DPT.
It is not infrequent to evaluate an individual seeking treatment for dizziness and for the patient to initiate the discussion of their symptoms with a disclaimer: “you are going to think I am crazy.” Shortly thereafter comes a frequently spoken concern: “I fear that physical therapy and exercise are only going to make my dizziness worse.” Such concerns are followed by “I didn’t think anything could be done to treat my dizziness.”
Dizziness increases one’s risk of falling, leads to decreased physical activity, causes one to cancel social outings, creates a fear of leaving the home, interferes with family relationships, and exacerbates anxiety. It is important to realize that dizziness is not normal. Furthermore, there are things that can be done to manage and treat symptoms of dizziness.
Such disclaimers and concerns are what inspired us to host a 90-minute discussion last week on the role of physical therapy in treating and managing dizziness. Special thanks to everyone who came out to Langford Sports & Physical Therapy for our evening conversation. For those of you who were unable to make it, read on for a few pointers to help you, a friend, or a family member managing symptoms of dizziness.
What is dizziness?
It can be difficult to describe dizziness and the range of symptoms can be diverse. Being “dizzy” may mean: woozy, ungrounded, nauseas, lightheaded, room spinning, imbalanced, unsteady, motion sensitive or about to pass out. Describing dizziness can be hard.
The vestibular system
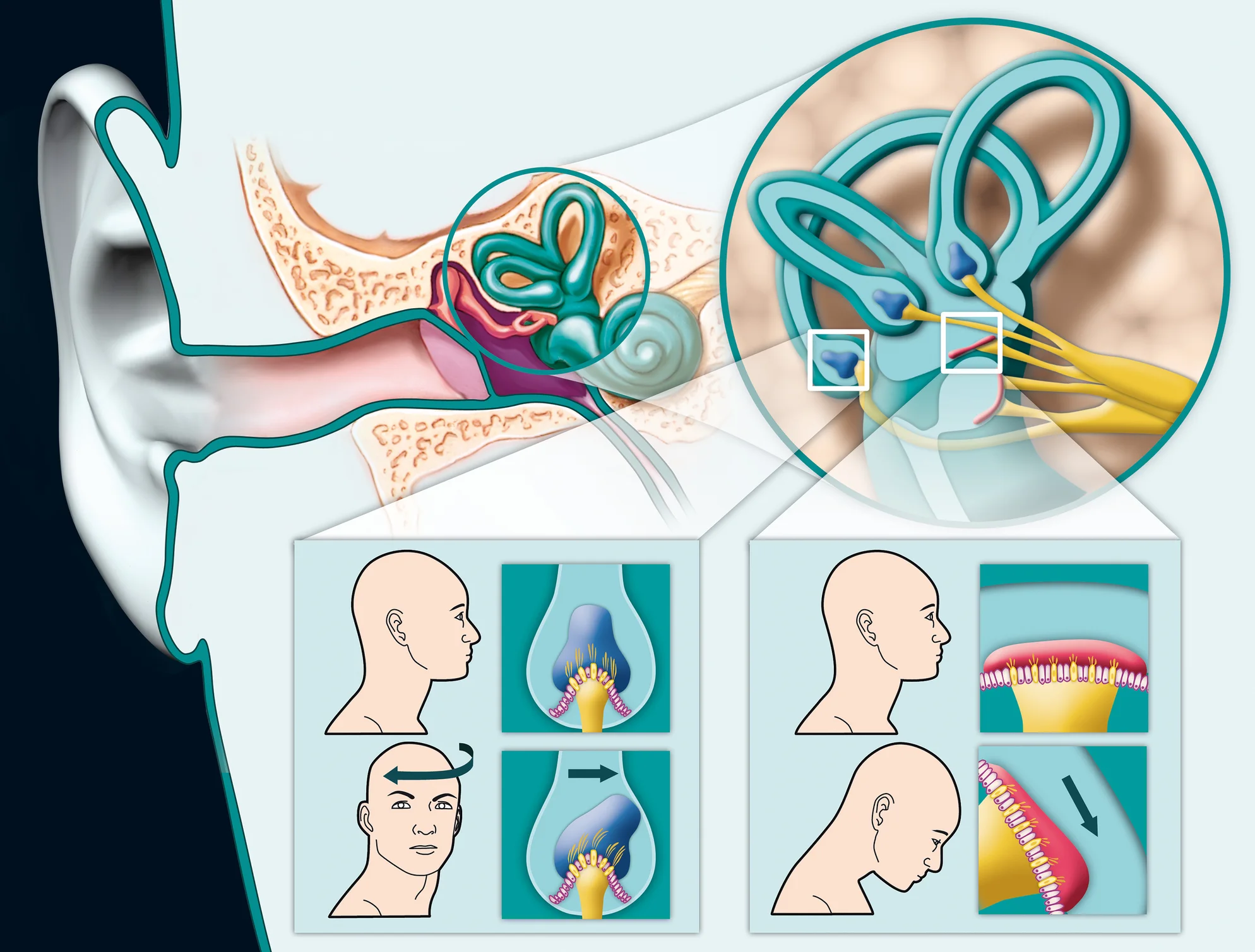
Dizziness is frequently caused by misinformation coming to the brain from the vestibular system, part of the inner ear. The vestibular system, also known as the balance organ, is located deep enough inside the ear that it cannot be seen during a basic physical exam. This system includes the labyrinth (3 semi-circular canals and ampulla) and the otolith organs (the utricle and saccule).
Photo by Dissoid/iStock / Getty Images
The semi-circular canals
Your canals are filled with a fluid called endolymph. With rotational movement (side to side rotation and up/down nodding), this fluid moves and activates the vestibular nerve. This activation sends signals to the eye and to the brain that keep our vision focused when the head is moving and keep us upright, balanced, and stable.
The otolith organs
These organs sense linear acceleration and tilt. Otoliths are calcium carbonate crystals that rest on a membrane with hair cells. When the head tilts forward or to the side, these calcium carbonate crystals move on the membrane, sending a signal to the eyes and brain that our head is tilting. This helps our brain distinguish between tilt of the head and tilt of the entire body. The otolith organs also help us sense acceleration, such as when we are sitting a red light and the vehicle next to us starts moving forward. The otoliths helps us realize we are still; we are not rolling backward.
When should I see a doctor or a physical therapist?
Physical therapy is appropriate for individuals experiencing dizziness that is caused by misinformation coming to the brain from the vestibular system. Symptoms of vestibular dizziness include sensations of room spinning, unsteadiness, imbalance, nausea, motion sensitivity, drifting with walking, ungrounded, and fatiguing eyes.
Benign Paroxysmal Positional Vertigo (BPPV) is caused when the calcium carbonate crystals of the otolith organs are misplaced and fall into the semi-circular canals. Symptoms of BPPV include brief spells, typically lasting less than one minute, of room spinning vertigo that is triggered by changes in position. There is a 67-81% chance that BPPV can be treated by a physical therapist within 2 visits.
A vestibular hypofunction is when the left ear and right ear vestibular systems are sending different information to the eyes and brain. There are numerous causes for a hypofunction including infection, toxicity from some medications, brain injury, Meniere’s disease, MS, and some surgical procedures in the vicinity of the ear. Many causes of a vestibular hypofunction are unknown. Symptoms of a hypofunction include dizziness with head movements and turning the body, such as rounding a corner; imbalance; unsteady; drifting while you walk; woozy; motion sensitivity. Research and clinical experience indicate that vestibular rehab with physical therapy is safe and effective for treating symptoms and improving function for individuals with a vestibular hypofunction.
Dizziness can also be caused by the neck, this is called cervicogenic dizziness. Your physical therapist will consider the neck as a contributing factor to your dizziness if you have a history of neck pain, difficulty moving your head and neck, wooziness, unsteadiness, and difficulty with imbalance.
The vestibular does not cause disturbed speech, difficulty swallowing, double vision, difficulty with coordination, facial droop, or a sensation of passing out. If you are experiencing these symptoms, it is important to seek medical attention right away.
Do all physical therapists treat dizziness?
We have two physical therapists at Langford Sports & Physical Therapy who have advanced training in treating the vestibular system. We are also fortunate that our PTA is also trained in vestibular rehabilitation. All of our physical therapists have some knowledge of the vestibular system and dizziness, but most complex cases are treated by those with more advanced training. Give our clinic a phone call for an evaluation if you are experiencing dizziness and have further questions!
How do I make an appointment?
Contact our front office today to schedule an evaluation. You may not need to see a doctor prior to being evaluated by your physical therapist, depending on your insurance. Call today and see if physical therapy can help you with your dizziness and balance.
Now what? Keep up to date and catch the details you missed with our blog.
In case you were overwhelmed by the amount of information that was presented, follow our blog online or find us on Apple News for regular updates. Our next article will have some exericises you should include in your training program to reduce your risk of injury.
Thank you again, and please be sure to swing back in, either to see a PT for an injury, work with Julie for an injury risk screening, or to try a MovNat class or run on the AlterG.
This blog was written by Dr. Karen Lovely, PT, DPT. Dr. Lovely received her Doctorate in Physical Therapy in 2016 from the University of Wisconsin-Madison. She enjoys practicing as a generalist, working with a variety of patients with orthopedic injuries and neurological disorders. She particularly enjoys working with recreational athletes and older adults. Karen is also trained to treat patients with dizziness, vertigo, and balance impairments.